
Introduction
For hospitals with more than 250 beds, annual laundry costs average $1.7 million — ranking among the top non-clinical budget line items after staffing. The average facility processes 12–18 lbs of linen per patient day, meaning laundry volume scales directly with census.
Whether to run laundry on-premise or outsource it can shift annual operating budgets by hundreds of thousands of dollars. With labor alone accounting for nearly 50% of on-premise laundry costs and commercial laundries claiming 34–40% lower production costs, the numbers don't tell a simple story. This article breaks down the full financial picture — capital costs, staffing, compliance, and long-term flexibility — so hospital administrators can make the call with confidence.
TLDR
- On-premise laundry carries high upfront capital costs ($500K–$2M for a 200-bed hospital) with long-term cost control in return
- Outsourced laundry trades capital expenditure for recurring pay-per-pound service fees
- Volume above 15,000 lbs/week typically tips the math toward on-premise — hospital size and capital access matter too
- Hidden costs differ by model: depreciation and turnover (on-premise) vs. rate escalations and linen loss (outsourced)
- Modern automation technology has improved on-premise ROI, with labor reductions of 35–77%
On-Premise vs Outsourced: Quick Financial Comparison
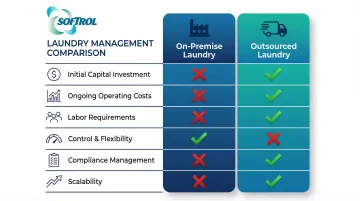
The table below breaks down the six most consequential financial and operational factors hospitals weigh when choosing between on-premise and outsourced laundry. Use it as a starting reference before diving into the full cost analysis.
| Factor | On-Premise Laundry | Outsourced Laundry |
|---|---|---|
| Initial Capital Investment | $500,000–$2M+ for equipment, facility construction, and infrastructure | $0 – No capital expenditure required |
| Ongoing Operating Costs | Labor (50% of budget), utilities, chemicals (5–10%), maintenance | Per-pound service fees, transportation charges, linen replacement |
| Labor Requirements | Specialized staff for operations, management, compliance, and maintenance | Minimal – vendor manages all processing labor |
| Control & Flexibility | Complete control over quality, schedules, and priority processing | Limited control; dependent on vendor schedules and capacity |
| Compliance Management | Hospital responsible for all regulatory compliance and audits | Vendor responsible; look for HLAC accreditation |
| Scalability | Fixed capacity; requires additional investment to expand | Variable costs scale with volume; easy to adjust |
What is On-Premise Laundry (OPL)?
On-premise laundry is a hospital-owned and operated facility located within or adjacent to the healthcare campus. The hospital invests in equipment, hires specialized staff, and manages all laundry operations internally, maintaining complete control over the entire processing cycle from soiled linen collection to clean linen distribution.
Core operational components include industrial washers and dryers, material handling systems, chemical dispensing equipment, quality control processes, and comprehensive staff training programs.
Modern facilities increasingly add automation technologies — rail systems, automated sorting equipment, and real-time tracking software — to improve efficiency and reduce labor requirements.
Financial Investment Requirements
Upfront Capital Costs:
- Facility construction or renovation with specialized ventilation and workflow separation
- Commercial laundry equipment purchase (washers, dryers, folders, ironers)
- Installation and utility infrastructure upgrades (water treatment, energy systems)
- Material handling automation and control systems
- Typical investment range: $500,000–$2M for a 200-bed hospital facility
Ongoing Operational Expenses:
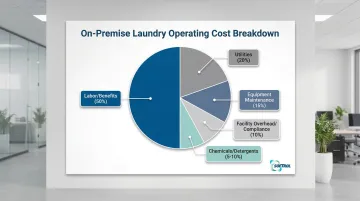
- Labor costs (wages, benefits, training) – approximately 50% of operating budget
- Utilities (water, electricity, gas) – commercial facilities spend 35–47% less per pound due to scale
- Chemicals and detergents – typically 5–10% of operating costs
- Equipment maintenance and repairs – OPLs spend roughly 58% more per pound than commercial facilities
- Facility overhead and regulatory compliance costs
The median hourly wage for laundry workers in hospitals was $16.86 in 2022, with total labor and benefits representing the largest expense category for on-premise operations.
Operational Advantages
On-premise operations provide complete control over quality standards, processing schedules, and turnaround times. Hospitals can prioritize critical items like surgical linens or isolation unit materials, ensuring availability exactly when needed. This control eliminates dependency on external vendors, reducing risks of service disruptions, delivery delays, or vendor business failures.
Modern automation has reshaped the OPL cost equation in meaningful ways:
- Automated sorting systems have documented labor reductions of 77% in healthcare laundries
- Productivity monitoring has increased operator efficiency by 35% within four months
- Single-operator management becomes viable at throughput rates up to 13,500 lbs/hr
These gains directly address the labor-heavy cost structure that has historically made outsourcing look more attractive on paper.
Operational Challenges
Despite automation gains, OPL operations carry real management burdens:
- Staffing: Hiring and retaining qualified laundry workers in a tight labor market requires ongoing effort and competitive wages
- Regulatory compliance: OSHA, CDC, and state agency requirements demand continuous investment in training, PPE, and audits
- Equipment reliability: Breakdowns can halt operations, requiring either in-house maintenance expertise or expensive service contracts
Space requirements present opportunity costs. The physical footprint needed for laundry facilities—often 40,000–86,000 square feet for larger operations—could potentially be used for revenue-generating clinical services. This trade-off becomes particularly significant in urban hospitals where real estate carries premium value.
What is Outsourced Laundry?
Outsourced laundry involves contracting with a commercial laundry service provider that picks up soiled linens from the hospital, processes them at an off-site facility, and delivers clean linens back on a scheduled basis. Service agreements typically span 3–5 years, with pricing based on weight processed or per-item costs, including pickup and delivery logistics.
Commercial laundries serve multiple healthcare clients, achieving economies of scale through high-volume processing and specialized equipment investments that individual hospitals cannot match.
Financial Structure
Cost Model:
- No upfront capital investment required
- Pay-per-use or subscription pricing based on pounds processed
- Costs scale directly with volume
- Typical contract elements include base service fees, transportation charges, and price escalation clauses (often 3–5% annually)
Pricing Options:
- Customer-Owned Goods (COG): Hospital owns linen, pays only for processing
- Rental Service: Vendor owns and replaces linen, charging a premium but eliminating hospital's inventory management burden
Commercial laundries can operate with 34–40% lower plant production costs per pound compared to on-premise facilities, primarily through labor efficiency, energy optimization, and maintenance economies of scale.
Operational Advantages
Outsourcing shifts the management burden — equipment maintenance, staff training, and regulatory compliance — to the vendor. Hospitals can verify processing standards through Healthcare Laundry Accreditation Council (HLAC) certification rather than managing compliance internally.
The variable cost structure also provides flexibility for hospitals experiencing census fluctuations or seasonal demand changes, with expenses scaling naturally with patient volume.
Operational Challenges
Outsourcing introduces trade-offs hospitals need to account for before signing:
- Reduced control: Quality, turnaround times, and urgent item prioritization depend entirely on vendor performance
- Service disruptions: Transportation delays, vendor labor issues, or facility problems can leave hospitals short on clean linen
- Contract lock-in: Multi-year agreements with 3–5% annual escalation clauses compound costs, and mid-contract exits often carry penalties
- Regional dependency: If a vendor becomes the sole provider in your area, renegotiating terms gets significantly harder
- Transportation overhead: Fuel surcharges, delivery scheduling, and on-site storage requirements for both soiled and clean linen add ongoing management complexity
Financial Analysis: Which Model Saves Money?
Determining which model saves money requires calculating Total Cost of Ownership (TCO) over a multi-year period:
On-Premise TCO = (Capital Investment ÷ Useful Life) + Annual Operating Costs + Hidden Costs
Outsourcing TCO = Annual Contract Fees + Transportation + Linen Replacement + Hidden Costs
The financial winner depends on several critical variables: laundry volume, available capital, facility efficiency, and long-term strategic priorities.
Break-Even Analysis
The break-even point occurs where cumulative on-premise costs equal cumulative outsourcing costs, typically within 3–7 years depending on volume and operational efficiency.
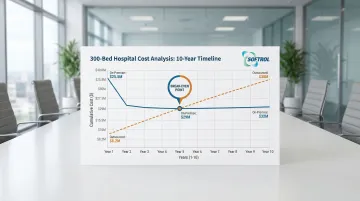
Sample Calculation for 300-Bed Hospital Processing 10,000 lbs/week:
On-Premise Costs:
- Initial capital investment: $1,500,000
- Annual operating costs: $400,000 (labor, utilities, chemicals, maintenance)
- Equipment useful life: 15 years
- Annual capital amortization: $100,000
- Total annual cost: $500,000
Outsourcing Costs:
- Processing rate: $0.85/lb
- Annual volume: 520,000 lbs (10,000 lbs/week × 52 weeks)
- Base annual cost: $442,000
- Annual escalation: 3%
- Year 1: $442,000 | Year 5: $497,000 | Year 10: $578,000
Break-even occurs around Year 5, when cumulative costs converge. After Year 5, on-premise operations generate a widening cost advantage — provided volume holds steady and major equipment replacements are planned for in the capital budget.
Hidden Costs: On-Premise
Equipment Depreciation & Replacement:
- Major laundry assets have 10–15 year useful lives
- Replacement cycles require significant capital reserves
- Technology upgrades needed to maintain competitive efficiency
Labor-Related Costs:
- Staff turnover averages 20% annually in laundry operations
- Ongoing training costs for compliance and equipment operation
- Benefits and payroll taxes add 30–40% to base wages
Operational Overhead:
- Utility rate increases compound over time
- Regulatory compliance audits and certifications
- Lost opportunity cost of space that could generate clinical revenue
- Management time diverted from core healthcare operations
Hidden Costs: Outsourced
Contract Escalation Compounding:
- Annual price increases of 3–5% compound significantly over multi-year contracts
- A $442,000 initial contract becomes $578,000 by Year 10 with 3% annual escalation
- Renegotiation leverage decreases once the vendor becomes entrenched
Transportation & Logistics:
- Fuel surcharges fluctuate with energy prices
- Minimum delivery fees regardless of volume
- Emergency delivery charges for urgent needs
Linen Loss & Damage:
- Linen loss rates can reach 15% without tracking systems
- Replacement costs range from $0.08–$0.20 per patient day
- Damage claims and restocking fees from vendor
Vendor Management:
- Staff time required to manage vendor relationships
- Quality monitoring and compliance verification
- Contract administration and invoice reconciliation
Volume Considerations
Laundry volume is the critical variable determining financial viability. Each volume tier tells a different story:
- High-volume (15,000+ lbs/week): On-premise economics improve with scale. Fixed costs spread across larger volumes, and automation investments become cost-justified.
- Low-volume (under 8,000 lbs/week): Outsourcing's variable cost structure wins. These facilities avoid underutilized equipment and can't match the labor efficiency of commercial operations.
- Seasonal swings: On-premise carries fixed costs through low-census periods; outsourcing costs scale down naturally. During peak demand, the equation flips — on-premise absorbs volume without per-pound increases, while outsourcing fees rise proportionally.

Long-Term Financial Projections
10-Year Cost Comparison:
On-premise costs stabilize after the initial investment. Operating expenses rise modestly with inflation and utility rates, but per-pound costs drop as volume grows — and automation upgrades in labor-intensive areas can reduce costs further over time.
Outsourcing costs compound with annual escalations. A contract starting at $442,000 reaches $578,000 by Year 10 with just 3% annual escalation — a 31% increase. On-premise costs over the same period typically rise only 15–20%, creating a cost gap that widens in favor of on-premise operations for high-volume facilities.
For most hospitals running above 10,000 lbs/week, the math tilts toward on-premise ownership somewhere between Years 3–7. The higher the volume, the earlier that crossover arrives.
Real-World Financial Impact: Hospital Case Study
Crown Health Care Laundry Services, a major healthcare laundry provider founded in 1955, demonstrates the financial impact of strategic automation investment. After successfully implementing Softrol's sortation and material handling systems at their 86,000 square foot Lakeland, Florida facility, Crown invested in a purpose-built, high-capacity processing facility in Atlanta, Georgia.
Atlanta Facility Implementation:
- High-volume continuous soiled laundry sorting system with 13,500 lbs/hr throughput capacity
- Automated weight registration and sling change-out capabilities
- Main storage capacity of 25,000 lbs across 12 rails
- Integrated clean storage with automatic delivery to finishing use points
Financial Outcomes: Those system capabilities translated directly into measurable cost improvements. Similar implementations at other healthcare laundries have documented:
- 77% reduction in sorting labor while processing 3,500 garments per hour
- 35% increase in operator productivity (Pounds Per Operator Hour rising from 90 to 140) within four months
- Payback periods of 2 years for automation investments

Key Takeaways: Financial outcomes depend on hospital-specific variables: processing volume, available capital for automation investment, and operational expertise.
Facilities processing high volumes (15,000+ lbs/week) that invest in modern automation can achieve on-premise economics competitive with — or superior to — outsourcing, while retaining the operational control healthcare environments require.
Frequently Asked Questions
What is OPL laundry?
OPL (On-Premise Laundry) refers to hospital-owned facilities where all linen processing happens on-site. It's typically chosen by larger hospitals processing 15,000+ lbs/week that prioritize control over quality, turnaround times, and can support the capital investment.
What is the difference between insource and outsource?
Insourcing means the hospital owns and operates its laundry facilities — higher upfront capital, but full operational control. Outsourcing contracts that work to an external provider, eliminating capital requirements but reducing control over processing schedules and quality oversight.
What are the advantages of outsourcing hospital laundry?
Outsourcing eliminates capital investment requirements, converts fixed costs to variable expenses that scale with volume, and removes the burden of equipment maintenance and specialized staffing. Commercial laundries operate with 34–40% lower production costs through economies of scale.
What services do hospitals outsource?
Hospitals commonly outsource laundry, food service, environmental services (housekeeping), IT infrastructure, revenue cycle management, and billing operations. Laundry ranks among the most frequently outsourced non-clinical functions, with approximately 60% of hospitals using external providers for some or all textile processing.
How to manage linen in a hospital?
Hospital linen management follows a continuous cycle: collection from patient areas, transport to processing, cleaning per CDC protocols, and redistribution to clinical units. Modern facilities use RFID or barcode tracking at each stage, cutting linen loss rates from 15% to under 3%.
What are the three categories of hospital laundry?
The three categories are: soiled linen (non-infectious routine items), infectious linen (from patients with known infections), and isolation linen (from patients with communicable diseases). Each requires distinct bagging, labeling, and processing protocols per OSHA and CDC guidelines.


